Cases of dangerous bacterial infection on the rise in Mississauga and other parts of Ontario
Published May 31, 2023 at 4:44 pm
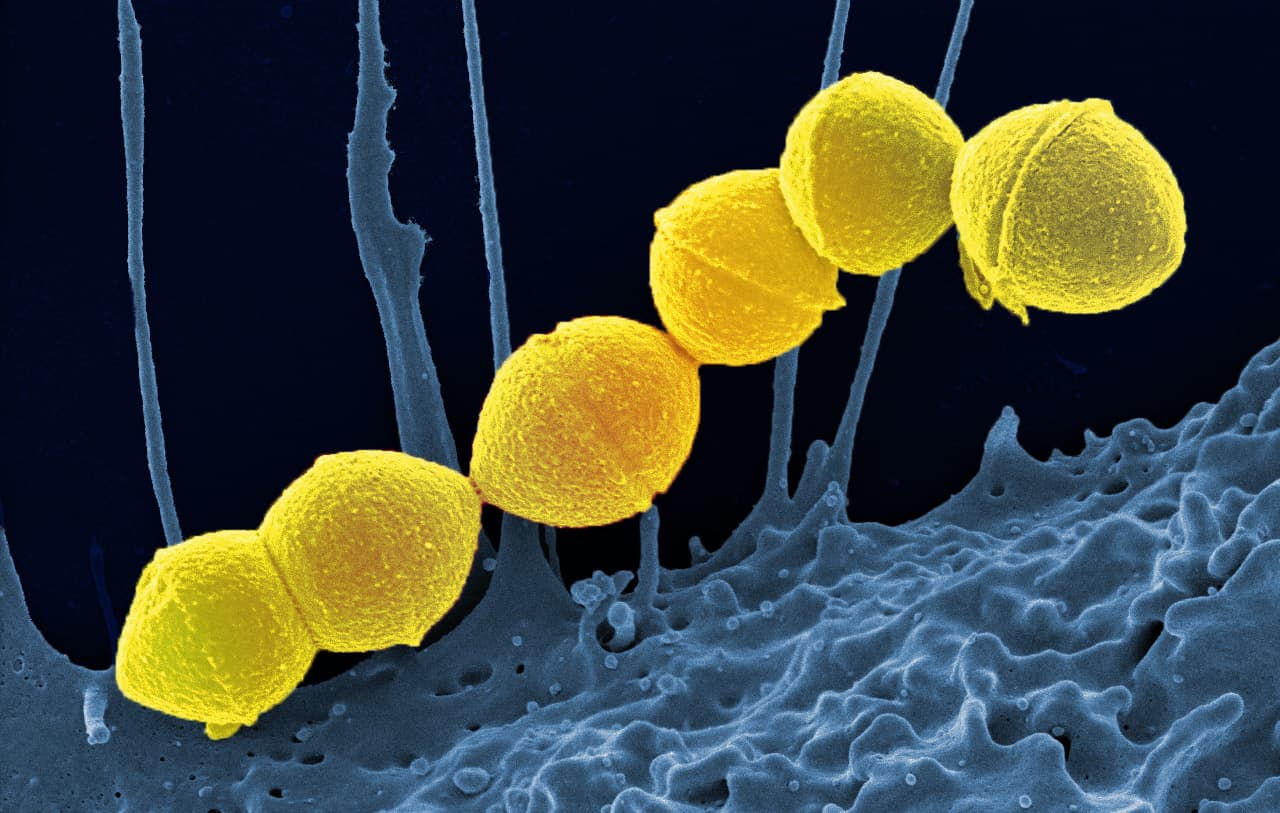
Health care experts in Mississauga, Halton and surrounding areas are warning people not to ignore a sore throat or skin infection that appears to be getting worse because although the chances of something being seriously wrong remain low, cases of a serious and potentially life-threatening bacterial infection are on the rise.
Earlier this month, Dr. Sumon Chakrabarti, an infectious disease physician at Trillium Health Partners in Mississauga, took to Twitter to ask other medical professionals if they were also seeing a rise in cases of invasive Group A streptococcus (iGAS).
Group A streptococcus (or GAS) bacteria are commonly found in the nose, throat and skin and can cause common infections (which are typically treated with antibiotics) such as strep throat, scarlet fever, impetigo and cellulitis. While these infections are generally mild, the bacteria can, in rare cases, enter the bloodstream, muscles or tissues and cause severe illness–including toxic shock syndrome and necrotizing fasciitis (flesh-eating disease). In some cases, iGAS can lead to death.
According to Halton Region Public Health, symptoms of iGAS may include fever, chills, headache, rapid breathing and increased heart rate, severe pain and swelling, redness around a wound, confusion or a flat red rash over a large area of the body.
Several doctors answered Chakrabarti’s tweet in the affirmative, and data from Peel Public Health and the Ontario Ministry of Health bears out his observation.
Peel Public Health told insauga.com that from January to April 2023, 30 confirmed cases of iGAS were reported in Peel (Brampton, Mississauga and Caledon).
“By comparison, the average number of confirmed iGAS cases historically seen at this same time of the year for the years 2018 to 2022 was 16,” a spokesperson said in an email.
“We have seen a steady rise in cases since January, with high case counts in March and April relative to historical numbers.”
Halton Region Public Health, which serves Burlington, Oakville, Milton and Halton Hills, has also seen an increase.
“The number of iGAS cases reported to Halton Region Public Health has increased compared to the same time in previous years,” a recent report reads.
“Some of these cases have resulted in death.”
Public Health Ontario has also noted an increase across the province.
According to a report, a total of 894 confirmed iGAS cases were reported in Ontario between Oct. 1, 2022, and April 30, 2023–an overall incidence rate of 5.8 cases per 100,000 people.
The report says the increase in cases was observed starting in January 2023, noting that cases in residents 18 and younger declined in April compared to March 2023.
The report says the total number of iGAS cases reported in April 2023 is the highest monthly case count reported since the 2014/15 season.
“Overall, the monthly number of iGAS cases reported from October 2022 to April 2023 exceeded the number of cases for the same months in each of the five pre-pandemic seasons, with the exception of October 2017 and January 2018.”
The report says cases in people 18 and younger have also been up over historical averages (with the exception of January and February 2018). That said, the report notes that since January, 83 per cent of cases have been seen in adults who are 45 or older. Three iGAS cases have been reported in patients under 18–two in March and one in April.
As for what’s causing the uptick, Chakrabarti says a number of factors are likely at play.
“It’s multifactorial and it has to do with us coming out of a pandemic and the resurgence of other things,” he says, adding that while iGAS remains rare, he’s seen a “definite uptick.”
“In normal infectious disease practice, you’d see it from time to time. The trend is the same across the province and country. Others are seeing this phenomenon.”
The rise in iGAS cases is not exclusive to Canada. The UK reported an uptick in iGAS deaths in the 2022/2023 season, with 60 deaths recorded within seven days of an iGAS infection diagnosis. The official government website says 38 per cent of the recorded deaths occurred in people 75 and older, and 17 per cent occurred in children 10 and under.
Over 30 deaths in children were recorded in the UK by January 2023.
Chakrabarti says he’s seeing iGAS in patients he wouldn’t normally observe the disease in, such as those living outside of higher-risk settings such as shelters or congregate living facilities where close contact is more common.
“There are outbreaks from time to time, but what’s striking is that it’s happening in multiple places at once. England is several months ahead of us in what’s happening with their pandemic outlook, and last winter, they were seeing a lot of iGAS there and like clockwork, we’re seeing it on this side of the Atlantic.”
As for what’s driving it, Chakrabarti says one factor could be the resurgence of viruses that circulated less frequently amid the crisis stage of the pandemic when social distancing rules were in effect.
Although iGAS remains relatively rare, it’s more likely to occur after a viral infection.
“There are multiple factors. There’s increased incidence of viral pharyngitis that makes your mucus membranes raw, which puts you at risk for a post-viral bacterial infection. There’s talk about a more virulent strain [of strep] that immune systems haven’t seen yet, so it can be a bit more severe upfront,” he says.
“People are seeing each other more now. There are a lot of things happening with the natural exchange of microorganisms and that’s an expected part of being in a society where people are together. It’s a perfect storm and I don’t expect it to last forever. Like any kind of epidemic, it burns hot and once immunity catches up, it goes down again. We’ll always see group A strep, but not at this level.”
Dr. Yasser Mansour, a pediatrician with Pediatric Urgent Care, a clinic with locations in Mississauga, Oakville and Toronto, says that it’s important to treat standard strep infections quickly to prevent more serious complications.
“We’ve seen an increase in Group A strep across all sites. The children [we treat] range from three to 17 years [of age]. Most come with sore throat, fever, typical symptoms. Sometimes there’s headache, malaise, fatigue, not eating, vomiting, lymph nodes enlarged in the neck. Many have signs of throat infection and we can do an instant test (swab) and we start them right away on antibiotics,” he says.
Mansour says strep is common among school children, most of whom will present with mild infections.
“It’s very contagious, it’s very infectious. It spreads in schools and in the house. If it’s not treated, it can have complications.
“Because we’re an outpatient clinic, we don’t see the really, really sick children. The gold standard treatment [for strep] is penicillin. If a throat culture comes back positive for strep, we insist on amoxicillin or penicillin treatment.”
Mansour also says he’s seen a lot of patients with scarlet fever.
“It’s an advanced and more complicated case of strep and the children tend to be sicker and have a diffuse rash all over their bodies.”
Mansour says that it’s imperative to start treatment for a common strep infection early and ensure all the medication is taken as directed–even if the patient or their child starts to feel better within a day or two.
“Once diagnosed, the 10-day antibiotic course must be completed. [Untreated] GAS can have serious complications for the heart and kidneys,” he says.
“We want to prevent rheumatic fever, which can damage heart valves. The only way to prevent complications is 10 days of penicillin or amoxicillin, or other antibiotics for patients with penicillin allergies. They cannot stop the course early.”
Chakrabarti says seeing a doctor promptly is important.
“If your kid has a sore throat, trouble swallowing and a fever, get them seen. Do common sense things like wash your hands and stay home when sick,” he says.
“The risk [of iGAS] is still very small and the overwhelming majority with strep do just fine.”
Chakrabarti says fast treatment can prevent poor outcomes.
“Even with iGAS, as concerning as it is, some cases are not as severe. Sometimes we find it in people’s bloodwork when they’re not feeling too sick and they get antibiotics and get better. People do get severe disease and die, but even among iGAS, those cases are rare.”
Much like Chakrabarti, Mansour believes the uptick in strep infections and other respiratory illnesses is related to pandemic lockdowns holding viruses at bay temporarily.
“After two years of the pandemic, all the viruses and bacteria were there but there was no exposure. Children who are now three and four years old were not getting any exposure, so we’re seeing a lot of infection because immunity has not been built up.”
As for how to prevent strep infections, Peel Public Health suggests practicing “respiratory etiquette” (such as covering your mouth and nose when you cough or sneeze), keeping your hands clean and covering up scrapes and cuts. The health agency also says parents can help prevent serious infections in children by getting them vaccinated for varicella (more commonly known as chickenpox), as it can increase the risk of a serious strep infection.
Varicella is included in the standard vaccinations offered to Ontario children.
Chakrabarti says it isn’t always possible to know why one person develops a life-threatening iGAS case and another doesn’t.
“In 13 years of practice, some people [I’ve seen who] got iGAS were perfectly healthy. You could not put your finger on why it happened. The vast majority of people with strep disease don’t have to come to the hospital because they’re not all that ill,” he says.
“Wash your hands when you get home. If your child is sick with a fever, don’t send them to school or daycare. If you have a kid with a skin condition, make sure you keep it under control.”
“This [uptick] is a phenomenon that we expect to normalize in the coming months.”
insauga's Editorial Standards and Policies advertising





